Weight Restoration for Anorexia Nervosa Peer Reviewed Scholarly Sources
- Review
- Open up Admission
- Published:
Olanzapine in the treatment of anorexia nervosa: a systematic review
The Egyptian Journal of Neurology, Psychiatry and Neurosurgery volume 56, Commodity number:threescore (2020) Cite this article
Abstract
Anorexia nervosa, with the highest mortality rate among psychiatric diseases, is characterized by low body mass index, fear of weight gain, and disturbed body prototype. Even though multiple drugs have been proposed for the treatment of anorexia nervosa, current treatment modalities include nutritional support and psychotherapy. In this written report, our aim is to analyze the efficiency and possible adverse effects of olanzapine, an atypical anti-psychotic drug, in the handling of anorexia nervosa. The studies investigating the efficiency and possible adverse effects of olanzapine in anorexia nervosa have been searched by using iii databases (Embase, PubMed, and Cochrane Library). DerSimonian-Laird random furnishings meta-analyses take been used in the statistical analysis. Upshot of olanzapine treatment in accordance with the duration and dosage of drug have been analyzed by the decision of 95% confidence intervals (p value < 0.05 is considered equally statistically significant). Despite the presence of some contradictory studies, olanzapine treatment has been plant benign in anorexia nervosa. In addition, analysis reveals that statistically meaning benign outcome of olanzapine treatment is used at loftier doses and for short elapsing. Possible side effects include neuroleptic malignant syndrome, hypoglycemia, and heart block in patients suffering from anorexia nervosa. Even though in that location is obvious need for more comprehensive further studies, electric current literature favors olanzapine treatment. The efficiency of olanzapine is considered to be related to changes in dopaminergic and serotonergic system in anorexic patients both in terms of neurotransmitter levels and receptor activity.
Introduction
Anorexia nervosa (AN), classified as an eating disorder past DSM-5 forth with bulimia nervosa and eating disorder non-otherwise specified, is characterized by body weight less than 85% of that expected for age and height, disturbances in body image, amenorrhea, and fear of weight gain [1, ii]. Incidence of AN has been reported equally 0.ix-2% in females and 0.3% in males which remained stable over the concluding l years except an increase in females between ages 15-24 [iii, four]. Comorbid psychiatric conditions including obsessive-compulsive disorder, major depression, and anxiety disorders have commonly been reported [five, half dozen]. AN is considered equally the psychiatric disease with the highest mortality rate mostly attributable to its organic outcomes [5, 6]. Current treatment guidelines for AN include nutritional support and psychotherapy such as cognitive remediation therapy (CRT), dialectical beliefs therapy (DBT), and psychodynamic psychotherapy that tin be delivered in inpatient or outpatient setting.
Many drugs have been proposed as a pharmacotheraupetic handling option for AN while none has been canonical past Us Food and Drug Administration. Major candidates are antidepressants, anti-psychotics, mood stabilizers, and anti-obesity drugs (i.e., orlistat) [7]. Rationale behind trial of those medications is the contradistinct serotonergic system in patients with AN which may be the primary pathophysiology [8,9,10,11]. Despite lack of sufficient show regarding efficiency and safety, they are widely prescribed mostly due to comorbid psychiatric atmospheric condition in the patients [12]. Bupropion has been associated with increased seizure risk in AN patients, thus, the use of buproprion is contraindicated. Additionally, the employ of monoamine oxidase (MAO) or tricyclic anti-depressants (TCA) has not recommended due to insufficient beneficial effects [7].
Olanzapine, an singular anti-psychotic inhibiting serotonergic (v-HT2) and dopaminergic (D2) system, has been utilized in the treatment of major depression and certain mood disorders including schizophrenia and bipolar disorder. Many trials of olanzapine in AN patients in combination with psychotherapy and nutritional support have been performed with promising outcomes. Known adverse effects of olanzapine are dizziness, orthostatic hypotension, hypercholesterolemia, hypertriglyceridemia, hyperglycemia, weight gain, actress-pyramidal symptoms, dry out mouth, hyperprolactinemia, and insomnia. In this literature review, our aim is to evaluate the efficiency and rubber of olanzapine treatment in patients with AN.
Methods
Literature search
Studies investigating the possible office of olanzapine in the treatment of anorexia nervosa have been searched past using three databases (PubMed, Cochrane Library, and Embase) by utilizing Medical Discipline Headings (MeSH) which are listed every bit follows "anorexia nervosa", "olanzapine" and "antipsychotic agents". Reference lists of each study have been further assessed to minimize the take chances of overlooking any relevant written report.
Study selection
Abstracts of the studies plant in the literature search take been analyzed by 2 authors independently in order to appraise their eligibility for literature review. Studies that fit to the inclusion criteria of our literature review accept further been analyzed. Details of the literature review and written report choice procedure have been demonstrated in Fig. one [xiii]. Inclusion criteria for commodity selection are equally follows:
- 1.
The study should be conducted with patients that are diagnosed with anorexia nervosa and treated with olanzapine.
- 2.
Participants of the studies should be diagnosed with AN according to DSM-Iii, DSM-III-R, DSM-Four, DSM-V, Russell, or ICD-10.
- 3.
The article should be published in a peer-reviewed journal between 2009 and 2019 in English language.
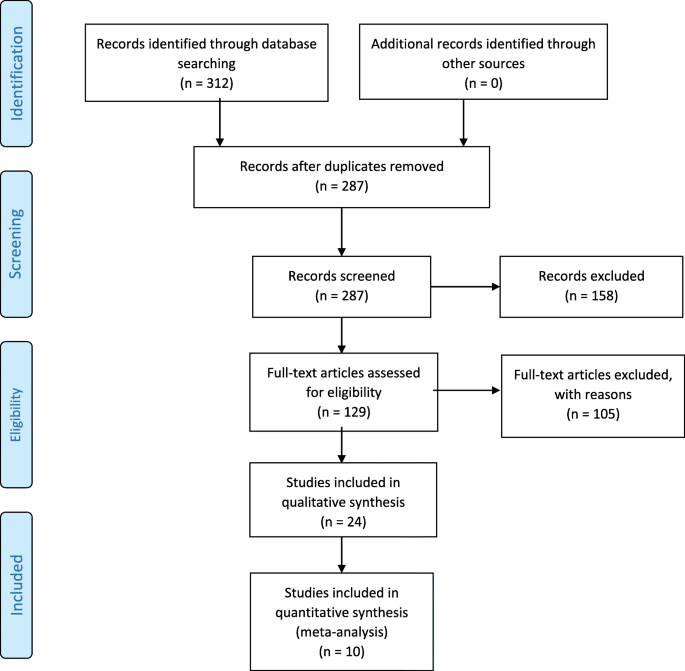
PRISMA flow diagram of the procedure of study selection for the systematic review [thirteen]
Quality assessment
Afterwards the decision of eligible studies, each study has been evaluated past both authors independently to appraise their "level of evidence" established by Melnyk at "Evidence-based practice in nursing & healthcare: a guide to best do" (criteria for level of evidence cess is available at Tabular array ane) [14]. In addition, each study has been farther assessed depending on the presence of the control group, size of study, participant selection criteria, presence of comorbid weather condition in the participants, consistency of data from each written report, and evaluation criteria for efficiency.
Statistical analysis
We used weighted mean difference (WMD) in guild to bespeak estimate each study which is an indicator of the treatment efficiency in terms of modify in body mass index (BMI) since studies analyzed in the review incorporate a variable number of participants [15]. We determined their 95% confidence intervals and their pooled effects by using DerSimonian-Laird random-effects meta-analyses as implemented in Comprehensive Meta-assay V ii.0 [sixteen]. T examination is implemented to compare the efficiency of treatment with the control groups.
Subgroup assay
We determined prior hypotheses for subgroup analysis in guild to analyze the possible source of differences among the written report results which includes trial duration (8 weeks or less vs. more than than 8 weeks) and dose of drug (low dose vs. high dose). We performed t test to assess the statistical significance of the differences and p value below 0.05 are considered equally statistically meaning.
Results
The literature review evaluates 24 studies comprised of 5 randomized controlled trials, eight instance-control studies, and 11 case reports (Table two). Amid them, a total of ten studies comprised of randomized controlled trials and case-control studies are plant eligible for statistical assay and quantitative evaluation.
Qualitative evaluation
Hansen (1999) demonstrated successful utilization of olanzapine, with an boilerplate of i kg/calendar week weight gain, in a 49-yr-old female patient with obsessive-compulsive disorder who received antidepressant handling before, including chlorpromazine [17]. A case series study with two patients suffering from anorexia nervosa over 5 years with multiple hospitalizations at the ages of 15 and 27 was the offset study exploring the efficiency of olanzapine in patients with no other comorbidities [18]. Both patients gained over 1 kg/calendar week (> iii% of their initial body weights), 1.2 kg/week, and 1.7 kg/week respectively, with v mg/mean solar day olanzapine handling [18]. Another instance serial written report demonstrating possible beneficial effects of olanzapine in the handling of AN included a fifty-twelvemonth-old female person without whatever comorbidity and a 34-year-old female with borderline personality disorder [19]. Later on, many other cases have been reported in adolescents and adults.
The first case-command study was performed in 2002 with 14 patients treated with 10 mg/mean solar day olanzapine for 10-calendar week period [21]. Ten patients gained 4 kg on average while the remaining four patients demonstrated a weight loss of approximately 1 kg [21]. The first randomized controlled trial comparing the efficiency of olanzapine versus chlorpromazine in AN patients illustrated no statistically pregnant difference in terms of weight gain [41]. Patients treated with olanzapine showed statistically less anorexic rumination behavior [41]. Withal, the primary limitation of this study is the lack of placebo control group [41]. Beginning placebo-controlled RCT performed in 2007 including 10 participants receiving olanzapine (two.five mg/day olanzapine for 2 months and 5 mg/day for four months) and 10 participants receiving placebo showed the inefficiency of olanzapine [24]. Both patient groups received behavioral therapy and nutritional support [24]. On the other hand, another placebo-controlled RCT performed with a total of 34 AN patients demonstrated a statistically significant beneficial upshot of olanzapine in terms of weight gain [25]. Patients receiving olanzapine demonstrated 4-indicate increase in BMI, on average, (standard deviation = 0.99) while the placebo group showed iii signal increment in BMI (standard deviation = i.32) [25]. Multiple other studies including case control and RCT have been performed over the terminal years with diverse outcomes.
Safe profile of olanzapine treatment in AN has also been a point of interest in our study. There are few case reports showing adverse effects including neuroleptic malignant syndrome, hypoglycemia, hyperglycemia, forenoon sedation, and heart block [34, 36, 37, 42]. However, most studies report no significant adverse reactions.
Quantitative evaluation
Weighted mean difference in BMI with olanzapine handling is 0.435 kg/m2 per calendar month (standard deviation of 0.139), whereas, WMD in BMI with the command group is 0.099 kg/m2 per calendar month (SD = 0.002). No statistically significant departure has been observed at the baseline BMI of command grouping and olanzapine group (p value > 0.05). Analysis of the effect of olanzapine on BMI compared to the control group reveals statistically significant beneficial effects (p value < 0.01; 95% CI: 0.316, 0.355).
Effect of therapy duration
WMD in BMI with brusk term olanzapine treatment (≤ eight weeks) is 0.477 kg/m2 per month (SD = 0.126) while WMD in BMI with long term olanzapine handling is 0.312 kg/m2 per month (SD = 0.143). Statistical assay regarding the duration of olanzapine therapy reveals that shorter duration of therapy is more benign (p value < 0.01; 95% CI: 0.12949, 0.20051).
Outcome of dosage
WMD in BMI with high dose olanzapine treatment (> five mg/day) is 0.499 kg/m2 per calendar month (SD = 0.12) while WMD in BMI with depression dose olanzapine handling is 0.295 kg/m2 per month (SD = 0.125). Statistical analysis regarding the dosage of olanzapine demonstrates that a college dosage of olanzapine is more beneficial (p value < 0.01; 95% CI: 0.17292, 0.23508).
Discussion
Anorexia nervosa, one of the eating disorders listed on DSM-V, is characterized by depression BMI, distorted trunk image, and extreme fear of weight gain that may lead to severe morbidity and mortality, specially among young females. Information technology is important to note that AN is considered to have the highest bloodshed rate among psychiatric conditions, thus, proper management is crucial. Currently, recommended therapeutic arroyo includes nutritional support and psychotherapy while there is no FDA-approved pharmacotherapy in the treatment.
Initial rationale backside olanzapine trial in AN patients is the side effect profile of olanzapine including weight gain and common comorbid psychiatric comorbidities of AN. Detection of lower levels of serotonin and its metabolite, v-hydroxyindolacetic acrid, in CSF along with contradistinct binding activities toward serotonergic receptors (5-HT1A and 5-HT2A) in patients with AN leads to trials of many anti-depressant and anti-psychotic drugs in AN treatment [8, ten, 24]. Additional findings regarding lower levels of dopamine and its metabolite (homovanilic acid) in CSF of AN patients along with altered bounden activities toward dopaminergic receptors (D2 and D3) provide supportive evidence [viii, 10, 24]. Although many other anti-depressant and anti-psychotic drugs take been investigated including risperidone, aripiprazole, fluoxetine, dronabinol, and alprazolam, olanzapine continues to remain equally the master candidate in AN treatment [43,44,45,46,47]. Furthermore, anti-psychotic drugs take shown to led an increase in serum leptin levels which may exist an additional beneficiary effect of olanzapine treatment in patients with AN [48].
Growing evidence indicates shared pathophysiological mechanisms betwixt schizophrenia and eating disorders including AN primarily from functional magnetic resonance imaging (fMRI) and neuroimaging studies [49, 50]. The primarily affected shared encephalon areas include inductive fronto-insular cortex and anterior cingulate cortex which are collectively referred every bit the salience network. Increased activation of the inductive cingulate cortex has been detected in AN patients while administration of sucrose solutions leads to decline in its activity as evidenced past fMRI findings [51]. Similar design of interest has been observed in patients with schizophrenia [52, 53]. Big scale meta-analyses demonstrate that anti-psychotic therapy is associated with alteration of activity of the salience network while following anti-psychotic therapy patients are more likely to have increased activation of the insular cortex when given static food-related images [54, 55]. Although the mechanism is not definitive with current literature and demand for further studies is clear, the potential benign effects of anti-psychotic therapy such as olanzapine in AN patients may exist underlined via correction of shared neurological circuit at the salience network.
Limitation of this review includes a low number of double-bullheaded randomized controlled trials, issues regarding the not-standardized duration of trials and dosages of therapy, and non-standardized therapeutic process. Although there is no articulate indicator of pick bias in the included studies and both olanzapine and control groups appear to have similar baseline features, possible selection bias in non-blinded studies should not be disregarded and should be considered equally some other limitation of this review.
To conclude, our findings support the utilization of olanzapine treatment in patients with AN by demonstrating a statistically meaning increase in BMI compared to placebo control groups with a relatively tolerable side effect contour. Nosotros detected that short term (≤ eight weeks) and higher doses (> v mg/twenty-four hours) of olanzapine treatment is more beneficial in terms of weight gain. However, there is a articulate demand for big calibration, more comprehensive studies regarding the efficiency and safety contour of olanzapine treatment in patients with AN in social club to have a ameliorate understanding of the subject area.
References
-
APA (American Psychiatric Association). Diagnostic and statistical manual of mental disorders-5th Edition (DSM-5). 2013; Washington DC, American Psychiatric Association.
-
National Constitute for Health and Care Excellence. Eating disorders: recognition and treatment. 2017.
-
Hoek HW. Incidence, prevalence and bloodshed of anorexia nervosa and other eating disorders. Curr Opin Psychiatry. 2006;19:389–94.
-
Keski-Rahkonen A, Hoek HW, Susser ES, Linna MS, Sihvola E, Raevuori A, et al. Epidemiology and course of anorexia nervosa in the community. Am J Psychiatry. 2007;164(8):1259–65.
-
Milos G, Spindler A, Schnyder U. Psychiatric comorbidity and eating disorder inventory (EDI) profiles in eating disorder patients. Tin can J Psychiatr. 2004;49(iii):179–84.
-
Ulfvebrand South, Birgegård A, Norring C, Högdahl L, Von-Hausswolff-Juhlin Y. Psychiatric comorbidity in women and men with eating disorders results from a large clinical database. Psychiatry Res. 2015;230(2):294–9.
-
APA (American Psychiatric Association). Practice guidelines for the treatment of patients with eating disorders (third ed.). 2016; Washington DC, American Psychiatric Clan.
-
Bailer UF, Frank GK, Henry SE. Exaggerated 5-HT1A simply normal 5-HT2A receptor action in individuals ill with anorexia nervosa. Biol Psychiatry. 2007;61:1090–10.
-
Brambilla F, Bellodi 50, Arancio C. Central dopaminergic role in anorexia and bulimia nervosa: a psychoneuroendocrine approach. Psychoneuroendocrinology. 2001.
-
Frank GK, Bailer UF, Henry SE. Increased dopamine D2/D3 receptor bounden afterwards recovery from anorexia nervosa measured by positron emission tomography and [11C] raclopride. Biol Psychiatry. 2005;58:908–12.
-
Kaye WH, Ebert MH, Raleigh M. Abnormalities in CNS monoamine metabolism in anorexia nervosa. Arch Gen Psychiatry. 1984;41:350.
-
Garner DM, Anderson ML, Keiper CD, Whynott R, Parker L. Psychotropic medications in adult and adolescent eating disorders: clinical practice versus evidence-based recommendations. Eat Weight Disord. 2016;21(iii):395–402.
-
Moher D, Liberati A, Tetzlaff J, Altman DG, The PRISMA Group. Preferred reporting Items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6:seven.
-
Bernadette M, Fineout-Overholt M, Fineout-Overholt E. Evidence-based practice in nursing & healthcare: a guide to all-time practise. 2005; ten.
-
Higgins JP, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat Med. 2002;21:1539–58.
-
DerSimonian R, Laird N. Meta-assay in clinical trials. Command Clin Trials. 1986;vii:177–88.
-
Hansen Fifty. Olanzapine in the handling of anorexia nervosa. Br J Psychiatry. 1999;175:592.
-
La Via MC, Grayness N, Kaye WH. Case reports of olanzapine treatment of anorexia nervosa. Int J Consume Disord. 2000;27(iii):363–six.
-
Jensen VS, Mejlhede A. Anorexia nervosa: handling with olanzapine. Br J Psychiatry. 2000;177(01):87.
-
Mehler C, Wewetzer C, Schulze U, Warnke A, Theisen F, Dittmann RW. Olanzapine in children and adolescents with chronic anorexia nervosa. A study of five cases. Eur Child Adolesc Psychiatry. 2001;10(2):151–7.
-
Powers PS, Santana CA, Bannon YS. Olanzapine in the treatment of anorexia nervosa: an open label trial. Int J Consume Disord. 2002;32(ii):146–54.
-
Ercan ES, Copkunol H, Çýkoðlu Southward, Varan A. Olanzapine treatment of an adolescent daughter with anorexia nervosa. Hum Psychopharmacol Clin Exp. 2003;18(5):401–3.
-
Dennis K, Le Grange D, Bremer J. Olanzapine use in boyish anorexia nervosa. Eating and Weight Disorders - Studies on Anorexia, Bulimia and Obesity. 2006; 11(2).
-
Brambilla F, Monteleone P, Maj M. Olanzapine-induced weight gain in anorexia nervosa: involvement of leptin and ghrelin secretion? Psychoneuroendocrinology. 2007;32(4):402–6.
-
Bissada H, Tasca GA, Barber AM, Bradwejn J. Olanzapine in the treatment of low body weight and obsessive thinking in women with anorexia nervosa: a randomized, double-blind, placebo-controlled trial. Am J Psychiatr. 2008;165(10):1281–8.
-
Low-dose olanzapine for anorexia nervosa. Brown University Child & Adolescent Psychopharmacology Update. 2010; 12(6).
-
Leggero C, Masi G, Brunori E, Calderoni S, Carissimo R, Maestro S, Muratori F. Low-dose olanzapine monotherapy in girls with anorexia nervosa, restricting subtype: focus on hyperactivity. J Kid Adolesc Psychopharmacol. 2010;xx(2):127–33.
-
Capasso A, Petrella C, Milano Westward. P.3.c.006 olanzapine in the treatment of anorexia nervosa: a instance study. Eur Neuropsychopharmacol. 2010;twenty:461.
-
Attia Eastward, Walsh B, Kaplan A, Yilmaz Z, Gershkovich M, Musante D, Wang Y. Olanzapine versus placebo for out-patients with anorexia nervosa. Psychol Med. 2011;41(10):2177–82.
-
Kafantaris V, Leigh E, Hertz South, Berest A, Schebendach J, Sterling WM, et al. A placebo-controlled pilot study of adjunctive olanzapine for adolescents with anorexia nervosa. J Child Adolesc Psychopharmacol. 2011;21(three):207–12.
-
Pirkalani Thousand, Anorexia N. P02-132 - successful treatment of 27 patients with anorexia nervosa with escalating doses of olanzapine citalopram loftier dose vitamin b6. Eur Psychiatry. 2011;26:728.
-
Bangratz S, Moyses M, Mader S, Huemer J, Koubek D, Laczkovics C, Karwautz A. Therapeutic drug monitoring of olanzapine in children and adolescents with anorexia nervosa: a pilot written report. Pharmacopsychiatry. 2012; 45(6).
-
Duvvuri Five, Cromley T, Klabunde M, Boutelle One thousand, Kaye W. Differential weight restoration on olanzapine versus fluoxetine in identical twins with anorexia nervosa. Int J Eat Disord. 2012;45(2):294–7.
-
Haruta I, Asakawa A, Inui A. Olanzapine-induced hypoglycemia in anorexia nervosa. Endocrine. 2014;46(3):672–3.
-
Kesic A, Lakic A. P.vii.d.003 olanzapine in treatment of adolescents with anorexia nervosa. Eur Neuropsychopharmacol. 2014;24:721.
-
Alwazeer A, Hussain A, Hickey A, Maclean D. Olanzapine associated heart cake in weight-restored anorexia nervosa. Prog Neurol Psychiatry. 2015;19(four):17–8.
-
Ayyıldız H, Turan S, Gülcü D, Poyraz C, Pehlivanoğlu E, Çullu F, et al. Olanzapine-induced atypical neuroleptic cancerous syndrome in an adolescent man with anorexia nervosa. Consume Weight Disord. 2016;21(ii):309–11.
-
Himmerich H, Dornik J, Bentley J, Schmidt U, Treasure J. Olanzapine handling for patients with anorexia nervosa. Can J Psychiatr. 2017;62(seven):506–seven.
-
Spettigue W, Norris One thousand, Maras D, Obeid N, Feder Due south, Harrison M, et al. Evaluation of the effectiveness and safe of olanzapine as an adjunctive handling for anorexia nervosa in adolescents: an open-label trial. J Tin Acad Child Adolesc Psychiatry. 2018;27(three):197–208.
-
Attia E, Steinglass J, Walsh B, Wang Y, Wu P, Schreyer C, et al. Olanzapine versus placebo in adult outpatients with anorexia nervosa: a randomized clinical trial. Am J Psychiatry. 2019;176(half-dozen):449–56.
-
Mondraty North, Laird Birmingham C, Touyz S, Sundakov Five, Chapman L, Beumont P. Randomized controlled trial of olanzapine in the treatment of cognitions in anorexia nervosa. Australasian Psychiatry. 2005;13(1):72–v.
-
Yasuhara D, Nakahara T, Harada T, Inui A. Olanzapine-induced hyperglycemia in anorexia nervosa. Am J Psychiatr. 2007;164(3):528–9.
-
Andries A, Frystyk J, Flyvbjerg A, Støving RK. Dronabinol in severe, indelible anorexia nervosa: a randomized controlled trial. Int J Consume Disord. 2014;47:18.
-
Frank GK, Shott ME, Hagman JO. The fractional dopamine D2 receptor agonist aripiprazole is associated with weight proceeds in boyish anorexia nervosa. Int J Eat Disord. 2017;5:447.
-
Hagman J, Gralla J, Sigel E. A double-bullheaded, placebo-controlled study of risperidone for the treatment of adolescents and young adults with anorexia nervosa: a pilot study. J Am Acad Child Adolesc Psychiatry. 2011;l:915.
-
Steinglass JE, Kaplan SC, Liu Y. The (lack of) effect of alprazolam on eating behavior in anorexia nervosa: a preliminary report. Int J Swallow Disord. 2014;47:901.
-
Walsh BT, Kaplan AS, Attia E. Fluoxetine later weight restoration in anorexia nervosa: a randomized controlled trial. JAMA. 2006;295:2605.
-
Ragguett R, Hahn K, Messina G, Chieffi South, Monda One thousand, De-Luca 5. Clan between antipsychotic treatment and leptin levels beyond multiple psychiatric populations: an updated meta-analysis. Hum Psychopharmacol. 2017;32:6.
-
Stip Due east, Lungu OV. Salience network and olanzapine in schizophrenia: implications for treatment in anorexia nervosa. Tin J Psychiatr. 2015 Mar;threescore(3 Suppl 2):S35–9.
-
McFadden KL, Tregellas JR, Shott ME, Frank GK. Reduced salience and default mode network activity in women with anorexia nervosa. J Psychiatry Neurosci. 2014;39(3):178–88.
-
Oberndorfer TA, Frank GK, Simmons AN, Wagner A, McCurdy D, Fudge JL, Yang TT, Paulus MP, Kaye WH. Contradistinct insula response to sweetness gustatory modality processing after recovery from anorexia and bulimia nervosa. Am J Psychiatry. 2013;170(x):1143–51.
-
Palaniyappan 50, White TP, Liddle PF. The concept of salience network dysfunction in schizophrenia: from neuroimaging observations to therapeutic opportunities. Curr Top Med Chem. 2012;12(21):2324–38.
-
Palaniyappan L, Liddle PF. Does the salience network play a key part in psychosis? An emerging hypothesis of insular dysfunction. J Psychiatry Neurosci. 2012;37(1):17–27.
-
Stip Due east, Lungu OV, Anselmo K, et al. Neural changes associated with appetite information processing in schizophrenic patients after xvi weeks of olanzapine treatment. Transl Psychiatry. 2012;2(vi):e128.
-
Leung M, Cheung C, Yu Yard, et al. Grey matter in beginning-episode schizophrenia before and after antipsychotic drug treatment. Anatomical likelihood estimation meta-analyses with sample size weighting. Schizophr Bull. 2011;37(1):199–211.
Funding
The authors declared no financial support.
Author information
Affiliations
Contributions
G.Ç.: Literature search and review, preparation of the manuscript, statistical assay. S.Ç.: Literature search and review, training of the manuscript, statistical assay. The writer(s) read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Approval from the Ethics Committee of Arel University has been obtained.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Boosted information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This commodity is licensed under a Creative Eatables Attribution iv.0 International License, which permits use, sharing, accommodation, distribution and reproduction in whatsoever medium or format, equally long as you requite appropriate credit to the original writer(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party textile in this commodity are included in the commodity's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted past statutory regulation or exceeds the permitted utilise, y'all will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/past/4.0/.
Reprints and Permissions
About this commodity
Cite this article
Çöpür, South., Çöpür, M. Olanzapine in the treatment of anorexia nervosa: a systematic review. Egypt J Neurol Psychiatry Neurosurg 56, lx (2020). https://doi.org/10.1186/s41983-020-00195-y
-
Received:
-
Accustomed:
-
Published:
-
DOI : https://doi.org/x.1186/s41983-020-00195-y
Keywords
- Olanzapine
- Anorexia nervosa
- Feeding and eating disorders
- Antipsychotic agents
- Body mass index
Source: https://ejnpn.springeropen.com/articles/10.1186/s41983-020-00195-y
Belum ada Komentar untuk "Weight Restoration for Anorexia Nervosa Peer Reviewed Scholarly Sources"
Posting Komentar